Addressing Breast Density with Your Patients

Washington has passed a new law requiring all patients who get a mammogram be notified of their breast density. Carol Milgard Breast Center will notify your patient of their breast density when they receive a mammogram result letter. Patients will be encouraged to have a conversation with you in this letter. The following key information should be helpful when communicating with your patients.
What is breast density?
As you know, a woman’s breast is composed primarily of two elements: fatty tissue and milk producing fibroglandular tissue. Breast density refers to the amount of fibroglandular tissue relative to fatty tissue in a woman’s breast. A woman is considered to have dense breasts if she has a lot of fibroglandular tissue and not much fatty tissue. Breast density tends to decrease with age and weight gain.
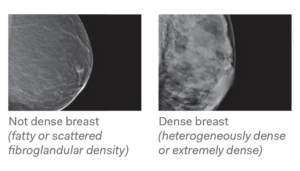
Why does breast density matter?
Women with dense breasts have an increased risk of breast cancer when compared to women with average or below average breast density. It is also more difficult to detect a small breast cancer on a mammogram in a woman with dense breasts.
What should I do if my patient has dense breasts?
Reassure the patient that breast density is only one small factor in determining breast cancer risk. Having dense breasts by itself does not increase a women’s risk for breast cancer. If a patient is found to be heterogeneously dense on her mammogram, her relative risk is 1.2 times above that of a woman with average breast density. If she has extremely dense breast tissue, her relative risk rises to 2.1 times above average. In a 50 year old woman, that translates to a ~5% 10 year risk of developing breast cancer.
What should I do if my patient requests additional imaging tests beyond screening mammography?
- If your patient has other risk factors such as family history, atypia on a previous biopsy or chest radiation, your patient would benefit from a breast cancer risk assessment. Patients with a lifetime risk above 20% could benefit from additional imaging evaluation beyond screening mammography. If the patients lifetime risk if greater than 20%, the patient should obtain annual screening mammograms and annual screening Breast MRIs. Screening MRIs are generally covered by insurance in high risk patients. If patient cannot undergo screening MRI, then screening Breast US is the best alternative.
- If your patient does not have other risk factors, screening mammography remains the best test to detect breast cancer in average risk women. Breast MRI and Breast US have the potential to find cancers not seen with mammography, but both detect significantly higher false positives, especially in average risk women. This can lead to a larger number of biopsies or follow-up examinations. In addition, both MRI and US are often times an out of pocket cost for an average risk woman. Discuss with your patient and decide on the best imaging tests to meet her screening needs. We advocate a shared decision making process.
Where can I get more information about breast density?
To speak with one of our radiologists, please call 253.759.2622 and follow the prompts. You can also visit the following websites for more information: www.wa-densebreastanswers.org.
